Everyone wins when family caregivers join the care team
At RubyWell, we’re helping family caregivers and Medicare Advantage plans work together to safely manage health at home. Including family caregivers on the care team can improve health outcomes and lower care costs for older patients with chronic illnesses.








Family Caregivers
27
Average # of hours family caregivers provide care each week
2 of 3
Family caregivers report moderate to high emotional stress

$1 trillion
Value of care family caregivers provide annually, most of it unpaid with no training or support

RubyWell has launched a study that provides eligible family caregivers with consistent support from a dedicated Care Navigator who acts as your personal guide through the healthcare maze. You’ll also get access to relevant training videos with info that can help you keep your loved one out of the hospital, saving both of you money, time, and heartache. And participation is free for family caregivers.
Managing medications, following doctors’ orders, getting your loved one to all of their medical appointments—the care you provide saves health plans money, too. That’s why RubyWell also compensates family caregivers enrolled in the study with a monthly stipend based on participation in study activities.

Older Adults
want to age at home safely
We’ve been hard at work helping families access the Medicare-covered home health services their eligible loved ones are entitled to. Care that’s proven to lower hospital readmission rates by up to 45%. Now we’re taking that model to the next level. By supporting, training, and providing a monthly stipend to family caregivers who participate in our study, we’re making it possible for older adults to spend more time at home and less in the hospital.
Home health care can save Medicare $17 billion annually. Read the full report
Health Plans
want to engage family caregivers
Acting as the care team’s boots on the ground, family caregivers have daily insight into your members’ health. And they’re usually the first to notice changes that could lead to an acute—and costly—care event.
RubyWell’s structured support and technology help family caregivers identify important health signals early and escalate them to the proper care provider in order to prevent avoidable hospital and ER usage.
Support where none existed
If you're caring for a homebound family member or friend, you may not have to do it all alone. Patients and their families love the support that RubyWell is helping them access.
Better health outcomes, lower costs
According to Medicare’s own data, home health care can keep homebound adults out of the hospital. That means families save money and time.
Home health care leads to better outcomes

Average hospital admits

90-day readmission rates
Tech you can trust
We take your privacy and safety seriously. Our systems keep your information secure and protect against fraud, waste, and abuse. We meet all HIPAA requirements and are SOC 2 Type II compliant, so you can feel confident your data is in good hands.


FAQs for Families
Yes, RubyWell’s new Family Caregiver study is designed specifically for family caregivers whose loved one is on Medicare, not Medicaid. If the person you care for lives in one of the counties we serve, and you’re both eligible for our study, you can get paid a monthly stipend based on your participation in study activities.
RubyWell’s study helps ease the strain of caregiving five ways:
1. Family Caregiver Support
We match you with a dedicated Care Navigator who can help guide you through the healthcare maze of doctors, health plans, and appointments. They’ll help coordinate all of your loved one’s care providers so you’re all on the same page. They’ll refer you to valuable resources in your community. You’ll meet with them virtually every week so they can get a sense for how you’re doing and if you need any help. You can also share concerns or questions with them at any time.
2. Training
We give you access to free training videos that are relevant to your loved one’s health condition and care needs. So you’ll learn the best ways to provide the care they need in order to avoid preventable trips to the hospital. You’ll also learn how to recognize changes in your loved one’s health that could suggest the need to escalate care. So you’ll know how to catch something before it becomes a dangerous health situation. The videos are short and pretty easy to fit into a busy schedule.
3. Community Building
You’ll join a cohort of other family caregivers in your area who are facing a lot of the same challenges you are. You’ll meet virtually every week, in a meeting facilitated by your Care Navigator.
4. Compensation
You’ll be paid a stipend of up to $300/month based on your engagement in study activities. Joining regular check-ins with the Care Navigator and your cohort, completing training videos, filling out regular check-in surveys, providing feedback on the study, and other study activities all count as engagement. If time is more valuable to you than money, you can choose to receive non-cash compensation, such as respite care or housekeeping assistance. The value of any non-cash compensation just can’t be greater than the value of the cash stipend you would be eligible to receive.
5. Medicare-covered home health services through JAA Home Health
The person you care for will receive professional home health services from JAA Home Health, a respected, Medicare-certified home health agency. This means a skilled nurse or therapist from JAA will bring medically-necessary care right to your loved one’s home. JAA Home Health is the only home health agency participating in this Family Caregiver Study. By enrolling in the study, your loved one is choosing to receive home health services from JAA.
No, there’s no cost for any of RubyWell’s services. Family caregivers already have enough expenses! And for Original Medicare (Parts A and B) beneficiaries, there’s no cost for any home health services they're eligible for. Original Medicare covers medically-necessary home health services for eligible patients.
Medicare Advantage plans (Part C) are required to cover the same services as Original Medicare, but they may charge a copay, and you may need prior authorization for care.
The free, online training videos we share with you range in length from 10 - 20 minutes each. So they’re easy to fit into a busy day. And they're packed with helpful information. At the end of each video, there are some questions you’ll need to answer to get credit for watching the video.
When you first join the study, you'll be asked to complete a series of initial training videos in order to start receiving support from your Care Navigator and participating in study activities that earn you monthly stipend payments. These videos walk you through topics like:
- How the program works and how we expect you to engage with us
- How to recognize changes in your loved one’s behavior or health that could lead to a health crisis
- When to call the home health agency vs. when to call an ambulance
Throughout the rest of the program, we’ll provide you with occasional training videos that are relevant to your loved one’s particular health condition(s) and care needs.
You’ll be matched with a dedicated Care Navigator for the duration of the study. Your Care Navigator is a social worker who has deep experience and expertise with helping aging adults and their family caregivers navigate the healthcare system. As an employee of our partner home health agency, The Jewish Association on Aging (JAA), the Care Navigator partners closely with the home health team to ensure seamless and frequent communication.
The support they provide includes:
- Facilitating multiple virtual “caregiver huddles” per week, when they will check-in with you on your loved one’s condition and your own needs or concerns as you provide care
- Coordinating early intervention and care transitions to help you prevent avoidable hospitalizations
- Following up with you after any hospitalization to support a smooth and safe transition back home
- Help with problem-solving and navigating to resources, planning next steps, and overcoming barriers to successful care
- Helping you understand what health signals to watch for and how to communicate concerns to the home health team
- Conducting home visits to help onboard you and your loved one to the study, build relationships, observe how care is provided and received, and help you navigate care pathways and resources
- Helping you understand and make the most of the support, training, and stipend payments available to you through this study
Family caregivers can receive a $300 stipend after successfully completing initial online training videos. Then they can receive a stipend of up to $300/month for continued participation in the 12-month program. The monthly stipend amount depends on the family caregiver’s engagement with regular check-in surveys, Care Navigator huddles, additional training videos, study feedback, and other study activities.
Home health care includes a range of medical and therapeutic services delivered in a patient’s home. Its goal is to promote, maintain, or restore health; slow a patient’s decline; or to help manage the effects of illness, injury, or disability.
Home health services are typically provided to patients whose health conditions make it difficult, impossible, or unsafe to leave their homes. They’re designed to ensure patients receive necessary care in a comfortable, familiar environment, out of hospitals or skilled nursing facilities.
Medicare covers home health services for beneficiaries who are homebound, at risk for future hospitalizations, and need assistance with activities of daily living (bathing, toileting, continence, dressing, eating, transferring).
Medicare considers a person homebound if both of these statements are true:
- They rarely leave home and when they do, it's just for short appointments or special events.
- Leaving home is difficult due to shortness of breath, pain, limited stamina, or other reasons.
And one of these statements is true:
- They require an assistive device (e.g., wheelchair, walker, crutches, cane), special transportation, or personal assistance to leave home due to illness/injury.
- Their doctor has recommended that they not leave home because of their condition.
Increase your census with Medicare patients
RubyWell helps Medicare-certified home health agencies identify patients who meet criteria as underserved community referrals, and streamlines the onboarding process.








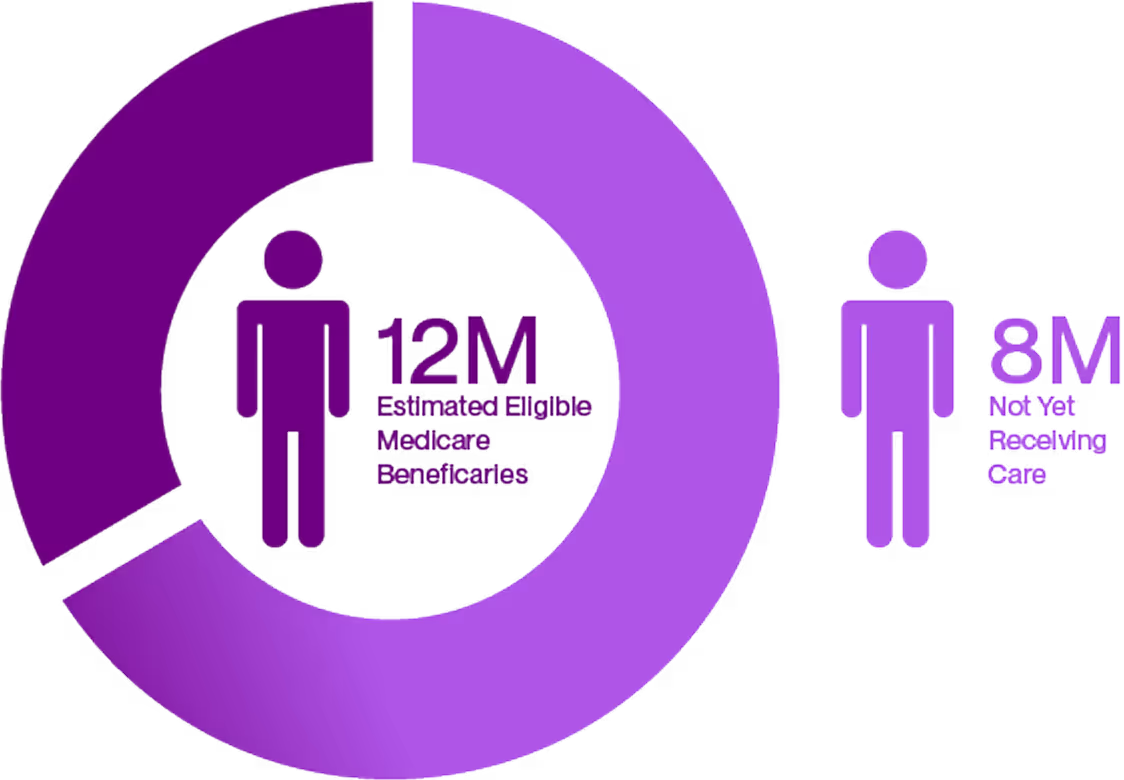
More care for more aging adults
An estimated 12 million Medicare beneficiaries are eligible for home health benefits, but only 4 million are receiving them. RubyWell helps eligible chronic patients on Original Medicare find their way to you.
Better health outcomes, lower costs
According to Medicare’s own data, families, healthcare providers, and Medicare win when eligible patients receive medically necessary home health services.
Medicare spending for non-home health users vs. home health users with similar conditions and risk factors
Inpatient
ER
SNF
Outpatient
Tech you can trust
RubyWell protects against fraud, waste, and abuse with rigorous audit practices. And we’re committed to maintaining the highest standards of security and data protection. As part of this commitment, RubyWell complies with HIPAA regulations and is SOC 2 Type II compliant.


FAQs for Partners
RubyWell reaches family caregivers of aging adults via advertising campaigns, organic content creation, and partnerships like NCOA and CAN. Our messaging shares information about the Medicare home health benefit and how we can help eligible patients access it. Families then choose to connect with us to learn more, check their loved one’s eligibility, and pursue care options.
We require the patient to share their Medicare ID number or photo of their Medicare ID card. We then run that information through a secure, third party insurance verification system called Stedi.
Our questionnaire asks several questions regarding the patient's mobility and the level of assistance they need to leave their home. We also ask how often they leave the home, and if their doctor has advised them not to leave home due to their health condition. Our information is verified on a follow-up phone call with every patient.


