The right care in the right place at a fraction of the cost
Families manage care decisions for your members at home daily. RubyWell provides the missing layer of cost-effective, continuous, structured engagement inside the home to help care teams reduce avoidable hospital admissions, ED visits, and SNF usage.
We’re launching a limited number of pilots with Medicare Advantage plans.

5% of members drive over 50% of healthcare spending
Managing the cost of members with complex chronic conditions is the greatest pain point in healthcare. They have 25% higher readmission rates and make up 78% of SNF patients. RubyWell gives value-based players a scalable way to capture early warning signs and intervene before costly crises occur.
Cost-Effective, continuous, structured engagement at home
Traditionally, the home has been the least connected and least supported part of the care system. Family caregivers provide the majority of day-to-day support. Yet their work is informal, clinically invisible, and uncoordinated.
RubyWell provides structured support to family caregivers, seamlessly connecting the home to the payer, leveraging existing infrastructure. This increases the plan’s care management reach and effectiveness inside the home.
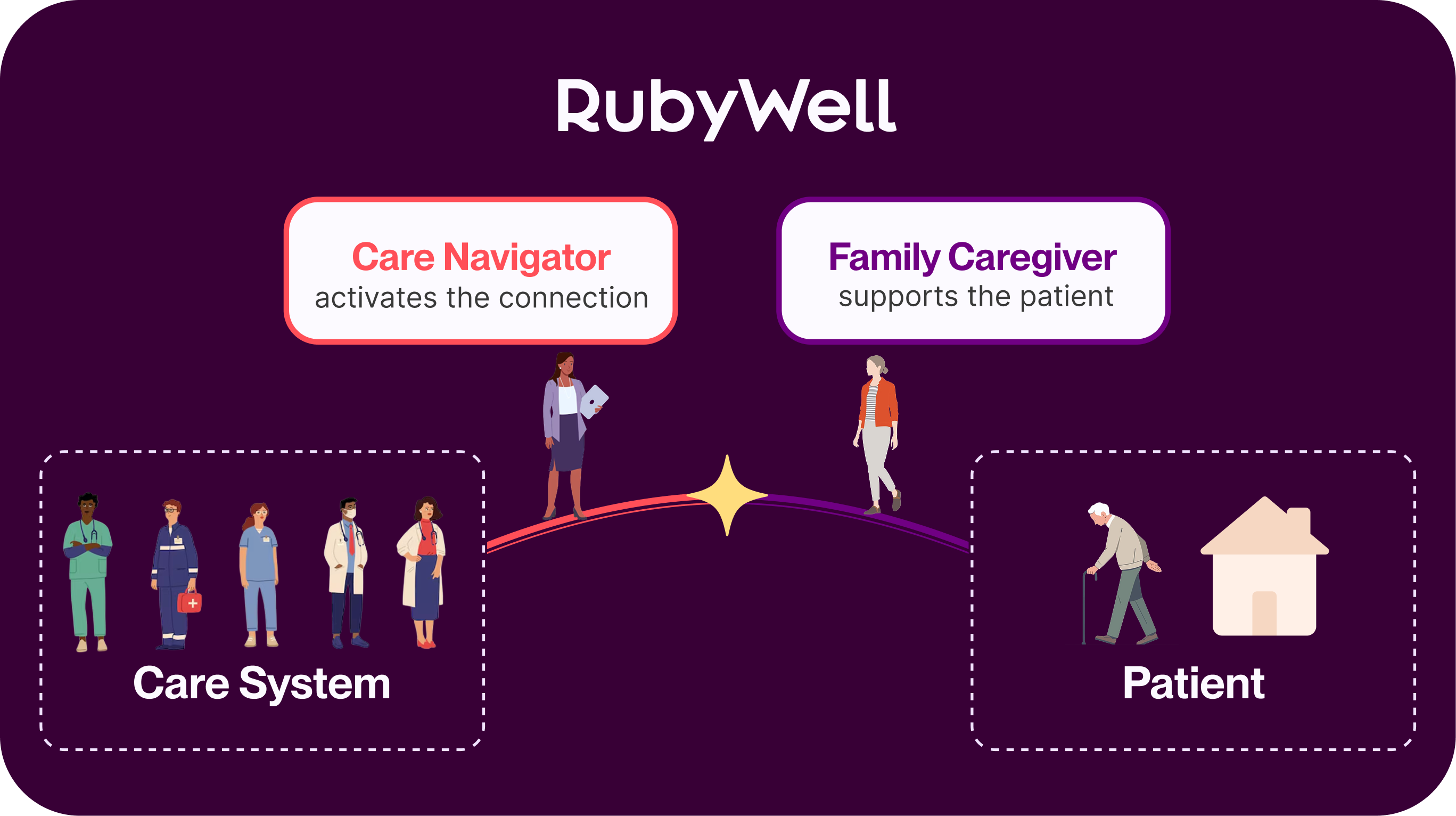
RubyWell works by amplifying existing care models
- It’s aligned to existing plan priorities and care pathways
- It offers flexible options for member enrollment
- Implementation is simple
We’re inviting a limited number of Medicare Advantage plans to partner with us in 2026.
Tech you can trust
RubyWell protects against fraud, waste, and abuse with rigorous audit practices. And we’re committed to maintaining the highest standards of security and data protection. As part of this commitment, RubyWell complies with HIPAA regulations, is SOC 2 Type II compliant, and is working toward HITRUST certification.


About RubyWell
RubyWell helps families and care teams work together to safely manage health at home.
CMS claims data show show that home health care improves patient outcomes and reduces healthcare costs. But home health visits tend to be brief and infrequent. Family caregivers provide the majority of support between visits, yet they’re often untrained, unsupervised, and disconnected from the care team.
Our proprietary technology and innovative approaches help plans, care providers, and families fill the gaps in the existing care system. This can improve patient outcomes, lower overall care costs, and ease family caregiver strain.



Health Plan FAQs
By reducing preventable hospital, ED, and SNF usage, RubyWell’s care model helps health plans reduce total cost of care (TCOC) for older adults with complex chronic conditions—your most expensive members.
For included members, RubyWell is designed to:
- Improve member satisfaction and retention
- Improve STAR-dependent metrics:
- 30-day re-admissions measure (triple weighted rating)
- Disease-specific measures (e.g. Diabetes, etc) - Improve physical health
- Reduce Total Cost of Care by right-sizing care
- Increase follow-ups after ED visits.
By reducing preventable hospital, ED, and SNF usage, RubyWell’s care model helps health plans reduce total cost of care (TCOC) for older adults with complex chronic conditions—your most expensive members.
As part of our standard model, RubyWell collects engagement data from the family caregiver via easy-to-use tools and LLM models. Self-reported family caregiver data includes:
- How they’re feeling while caring for the member
- Their confidence in understanding the care plan, day-to-day activities, and their ability to perform them
Quantitative metrics include:
- Call logs
- Survey questions
- Zoom participation
Qualitative insights are collected from:
- Care Navigator conversations
- Family caregiver sentiment
Data from this engagement and the Care Navigator “huddles” signal when additional support is needed.
We also collect the status of acute activity for care coordination purposes and to monitor progress that we compare against claims data on a quarterly basis.
When a clinical resource is engaged for real-time review, RubyWell may also collect real-time data like the member’s weight, blood pressure, A1C, etc. from the family caregiver. RubyWell is not a clinical decision support tool, and as such should only collect clinical data when appropriate resources are available for timely review and response, in coordination with our plan partners.
Additionally, RubyWell can collect inputs and encourage behavior that’s useful to the plan for administrative and/or clinical reasons. For example, while a family member cannot code for benchmark or close care gaps, they can provide information, schedule appointments, etc. as inputs to the plan so clinical resources can be deployed efficiently. This is particularly valuable to plans early in the enrollment year, when data about the member is not yet available.
Member dashboards that track this data collection are available through a portal interface to the plan.
RubyWell pays family caregivers a monthly stipend based on their engagement in program activities such as completing training videos, attending weekly check-ins with the Care Navigator and their caregiver cohort, participating in user surveys, interviews, and tests, etc. Alternatively, family caregivers can choose to receive non-cash compensation, such as respite care or housekeeping assistance. The value of any non-cash compensation cannot be greater than the value of the cash stipend they would be eligible to receive.
RubyWell is NOT structured as a benefit provided to the member, but rather a service that the plan is providing to lower costs.
RubyWell can work in various arrangements depending on the capabilities and availability of existing care management functions. In some cases, RubyWell entirely manages this function for enrolled members. In others, RubyWell may work only to connect the family caregiver with a plan-provided resource as the primary care navigation and management resource. More often, our Care Navigators bridge communication and action between families and plans, helping to coordinate these interactions as they do interactions with providers and other medical resources.
PCPs are critical to quality longitudinal care. We don’t aim to replace or sit between PCPs and families. Instead our goal is to make the relationship more productive and less burdensome for all involved. For example, our Care Navigators may prepare and send recent activity notes to the PCP ahead of a visit, or assist the family in making an appointment with the PCP.
In cases where PCPs already bear risk for the member, they’re likely the most excited to have additional support. We’re open to discussing different cost sharing models to make this successful for all involved.

